
Sharpen Your Clinical Skills: Diagnose and Manage Brugada Syndrome
An inherent cardiac disorder threatens the young, structurally healthy generation with sudden cardiac death.
According to the National Institute of Health (NIH), major reason for Brugada Syndrome (BrS) can be “autosomal dominant mutations in the SCN5A gene, which encodes a cardiac sodium channel, although other genetic and environmental factors may modulate disease expression.
These mutations impair sodium current, creating conduction abnormalities and predisposing to re-entrant arrhythmias.
The prevalence of the syndrome is estimated at around 15 per 10,000 in Southeast Asia, including Japan, and around 2 per 10,000 in the Western countries.
The BrS may be responsible for up to 4 % of all sudden cardiac deaths (SCD) and at least 20 % of SCDs in patients with structurally normal hearts.
It is 8–10 times more prevalent in males than in females, and males are at considerably higher risk of dying suddenly.
In Southeast Asia, the BrS is the leading cause of non-traumatic death in men younger than 40 years."
Fast Diagnosis Saves Lives
Changes in EKG help to offer implantation of a defibrillator to BrS patients.
BrS previously known as Sudden Unexplained Nocturnal Death Syndrome (SUNDS) can be identified with an appropriate diagnostic criteria recommended by the JACC (Journal of the American College of Cardiology):
Type 1 (Coved Type): An ST-segment elevation ≥2 mm in ≥1 right precordial lead (V1 to V3), followed by an rʹ-wave and a concave or straight ST segment.
The descending ST segment crosses the isoelectric line and is followed by a negative and symmetric T wave.
Type 2 (saddle-back type): ST-segment elevation ≥0.5 mm (generally ≥2 mm in V2) in ≥1 right precordial lead (V1 to V3), followed by a convex ST.
The r'-wave may or may not overlap the J point, but it has a slow downward slope.
The ST segment is followed by a positive T wave in V2 and is of variable morphology in V1.

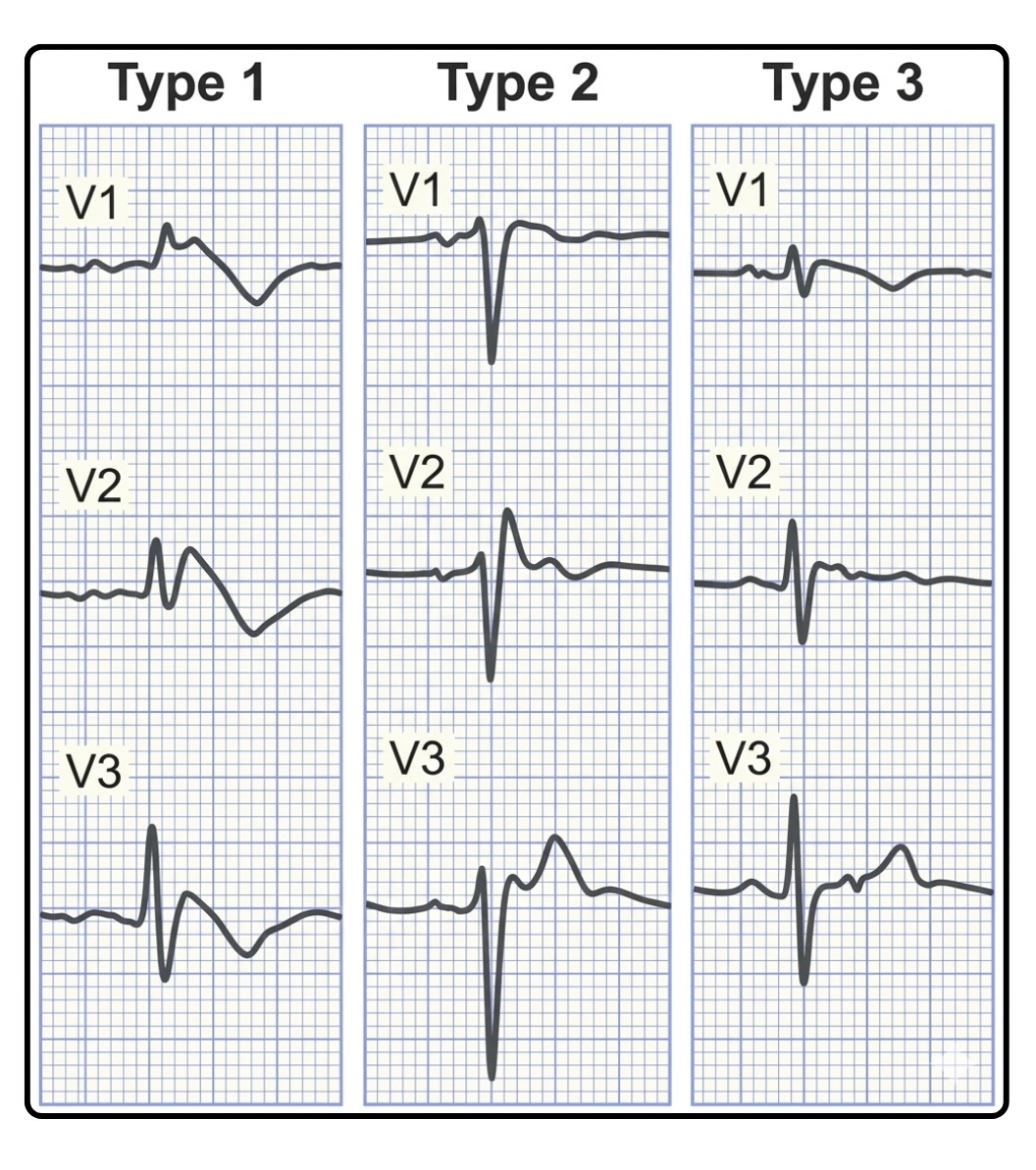
Many patients identified with Type 1 EKG remain asymptomatic.
The 2013 expert consensus statement defined Brugada Syndrome (BrS) as follows:
“BrS is diagnosed when a type 1 ST elevation is observed either spontaneously or after intravenous administration of a sodium channel blocker in at least one right precordial lead (V1 and V2), placed in a standard or superior position (up to the 2nd intercostal space).”.
Before confirming a diagnosis of Brugada syndrome, other potential causes of ST-segment elevation must first be ruled out.
An ECG pattern resembling Brugada syndrome type 1 that is induced by other underlying conditions is referred to as a Brugada ECG phenocopy.
Professional Learning & Training
APRN World helps RNs, APRNs, and other healthcare professionals enhance their EKG diagnostic and ECG interpretation skills through affordable, high-quality training programs.
Master arrhythmia recognition using APRN World’s EKG simulator.
It’s important to refer to expertly designed EKG and cardiac pharmacology guides, now available at AACN and Amazon at very low cost.










